Recovering from surgery involves more than just rest. It requires a structured physiotherapy programme designed to restore movement, strength, and overall function. Post-operative physiotherapy is essential in helping you regain your independence and safely return to daily activities.
Whether you’ve undergone a joint replacement, soft tissue repair, or another procedure, a personalised physiotherapy treatment plan can support your recovery and guide you towards better health. Understanding what to expect from your sessions reduces uncertainty and empowers you to take an active role in your rehabilitation.
This guide will walk you through the key stages of post-surgery rehabilitation, introduce the techniques your physiotherapist may use, and address common questions, ensuring you’re prepared for a smooth and effective recovery.

The Physiotherapy Process After Surgery
Post-operative physiotherapy is a carefully structured process designed to support your recovery throughout. From the initial assessment to goal setting and collaborative care, each stage is focused on helping you rebuild strength, regain movement, and restore confidence. Insights from clinical research on post-operative physiotherapy also guide many of these approaches, ensuring your programme is shaped by established principles in rehabilitation. Below, we’ll provide a detailed overview of what you can expect during this phase of your recovery.
Initial Assessment and Treatment Plan
The first physiotherapy session sets the foundation for your recovery journey. It’s an opportunity for your physiotherapist to gather essential information and understand your unique needs. Here’s what typically happens during this initial meeting:
Discussion about your surgery and medical history:
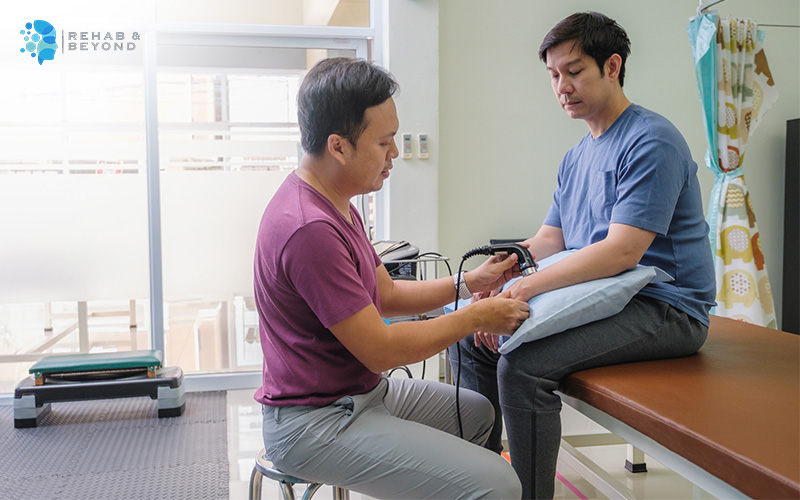
Your physiotherapist will ask about the type of surgery you’ve undergone, your overall health, and any pre-existing conditions that might influence your recovery. This allows them to gain a complete understanding of your situation.Inspection of the surgery site:
The incision area is carefully examined for signs of infection, swelling, or inflammation, which can affect your recovery timeline and influence the types of exercises introduced.Assessment of movement limitations:
Any movement restrictions, whether from surgical adjustments, muscle stiffness, or general weakness, are noted to identify areas that need priority.Creation of a personalised treatment plan:
Based on the gathered information, your physiotherapist will design a tailored, step-by-step plan, including musculoskeletal physio exercises and therapies, to help you overcome specific challenges and achieve your recovery goals.
Post-Operative Evaluation
The initial assessment goes beyond surface-level checks. It involves a thorough evaluation to identify both your strengths and areas for improvement.
Observation of movement patterns:
Your physiotherapist will observe how you walk, stand, and move to identify any compensatory behaviours, such as favouring one side of your body. These patterns can lead to imbalances that, if left unaddressed, may slow down your recovery.Testing joint range of motion:
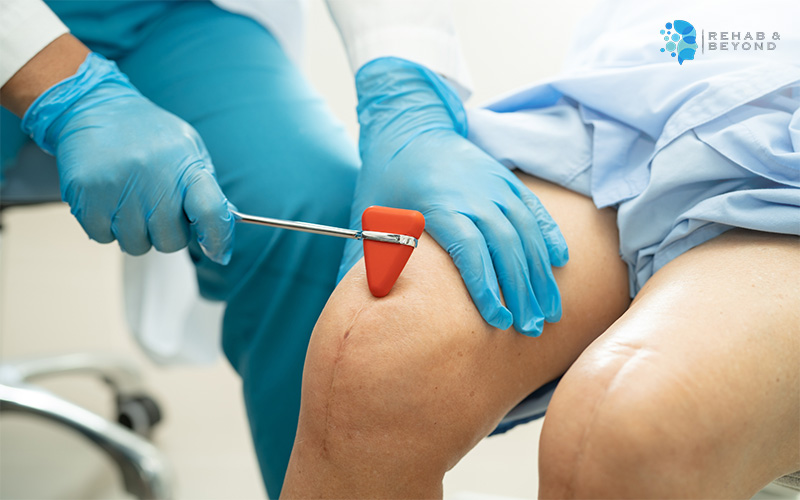
The physiotherapist will measure how far you can comfortably move the affected joints. This helps determine if there is stiffness or restriction that might require targeted stretching or mobilisation techniques.Assessing muscle strength:
The strength of the muscles surrounding the surgical site is tested, along with your overall body stability. Weakness in these areas can hinder recovery and increase the risk of re-injury.Evaluating pain levels:
Your feedback on pain, both during movement and at rest, is crucial. It helps your physiotherapist gauge the intensity of exercises and interventions, ensuring your rehabilitation progresses without unnecessary discomfort.
Goal Setting
Setting recovery goals gives your physiotherapy journey direction and purpose. These goals are created with your input to ensure they reflect your priorities and motivations.
Establishing clear objectives:
Your physiotherapist will help you define specific, measurable goals tailored to your recovery needs. For instance, you might want to regain full range of motion in your knee after joint replacement or reduce swelling and stiffness in the early stages of recovery.Breaking it down into milestones:
Long-term recovery can seem daunting, so goals are broken into smaller, more manageable steps. These milestones help you stay on track and motivated as you make progress.Focusing on full recovery:
While short-term goals are important, the ultimate aim is to restore your ability to engage in daily activities, hobbies, or sports with confidence and independence.
Collaborative Approach
Successful recovery depends on a partnership between you, your physiotherapist, and, when necessary, your support network.
Working together with your physiotherapist:
Open communication is encouraged so you can voice concerns, ask questions, and actively contribute to your treatment plan.Involving family or caregivers:
For those who need extra help at home, family members or caregivers can play a valuable role in assisting with exercises and tracking progress.Personalised and flexible care:
Recognising that every recovery journey is different, your treatment plan is adjusted as you progress, ensuring it continues to meet your evolving needs.
By combining professional guidance with active participation, post-operative physiotherapy provides a solid foundation for your recovery. Each session takes you closer to regaining your strength, mobility, and independence.

Rehabilitation Techniques Used After Surgery
Rehabilitation after surgery involves various physiotherapy techniques, each carefully chosen to address specific challenges. These methods are designed not only to aid recovery but also to restore function, improve mobility, and enhance overall well-being. If you are visiting a physiotherapy clinic in Singapore, you may encounter many of these approaches as part of your rehabilitation journey. Here’s an overview of some common techniques your physiotherapist may incorporate into your treatment plan.
A. Manual Therapy
Manual therapy is a hands-on approach aimed at relieving pain, reducing stiffness, and improving mobility in the affected area.
Massage:
Focused on easing muscle tension, improving blood flow, and alleviating pain around the surgical site, massage can help relax muscles, reduce swelling, and speed up recovery.Joint Mobilisation:
For patients experiencing joint stiffness or restricted movement, gentle manipulation of the joint is performed to restore normal motion, reduce discomfort, and support functional recovery.Soft Tissue Work:
Soft tissue techniques promote relaxation and prevent long-term restrictions in mobility by targeting areas of muscle tightness or knots that may develop post-surgery.
B. Exercise Therapy
Exercise is a cornerstone of post-operative rehabilitation, tailored to each stage of recovery to ensure gradual progress.
Initial Movements:
In the early days of recovery, gentle exercises such as ankle pumps, leg lifts, or arm stretches may be used to help maintain range of motion and prevent stiffness in the affected area.Strengthening Exercises:
As you heal, resistance exercises are introduced to rebuild muscle strength around the surgery site. These may include isometric holds, light weightlifting, or resistance band workouts, which progressively challenge and strengthen muscles.Coordination and Balance Training:
Exercises focused on proprioception, such as standing on one leg or balancing on an unstable surface, help restore coordination and stability, which are crucial for regaining functional movement and preventing falls.
C. Modalities and Other Techniques
Your physiotherapist may employ a combination of modalities to manage pain, reduce swelling, and accelerate recovery.
Heat Therapy:
Applying heat to the surgical site can help relax stiff muscles, increase blood flow, and alleviate discomfort, particularly in the early stages of physiotherapy.Cold Therapy:
Ice packs or cold compresses are effective at reducing swelling, numbing pain, and managing inflammation, especially immediately after surgery.Ultrasound Therapy:
This technique delivers deep heat to tissues, stimulating circulation, reducing inflammation, and speeding up the healing of muscles and ligaments.Electrical Stimulation (TENS):
Transcutaneous Electrical Nerve Stimulation (TENS) delivers mild electrical currents to block pain signals and stimulate muscle activation, especially useful for managing post-operative pain and strengthening weakened muscles.
D. Home-Based Physiotherapy
Home-based physiotherapy is an excellent option for patients who prefer convenience or face challenges in visiting a clinic.
Convenience for Patients:
Home-based therapy is particularly beneficial for individuals with mobility restrictions, transportation difficulties or those who feel more comfortable in their own environment.Consistency in Practice:
With physiotherapy at home, patients can maintain regularity in their exercises, helping to avoid gaps between clinic visits and ensuring steady progress.Integration with Daily Routines:
The physiotherapist will design a recovery programme that seamlessly integrates with your lifestyle. The programme will include exercises adapted to your home environment, making it easier to stay on track and achieve your recovery goals.
Post-operative physiotherapy combines various techniques to provide a comprehensive approach to recovery. Each method is tailored to your specific needs, ensuring a safe and steady path back to optimal health and function.

Monitoring Your Recovery Progress
Post-operative physiotherapy is a dynamic process, evolving as recovery progresses to meet the patient’s individual needs. Monitoring the recovery journey and adjusting the treatment plan are crucial for effective rehabilitation. Here’s how physiotherapists support progression and recovery:
Ongoing Evaluation
To keep the recovery process on track, physiotherapists perform regular assessments that provide insights into the patient’s progress.
Regular Check-ins:
Follow-up appointments offer valuable insights into the patient’s recovery, ensuring the plan remains aligned with current needs. These visits help identify any challenges early on.Movement Assessments:
Each session includes a reassessment of physical parameters such as range of motion, joint mobility, and muscle strength. This allows physiotherapists to monitor improvements and pinpoint areas needing further attention.Patient Feedback:
Open communication is encouraged throughout recovery. Patients are invited to share their experiences, pain levels, and discomfort, helping the physiotherapist adapt the plan to meet evolving needs.
Modifying the Plan
As recovery progresses, physiotherapists adapt treatment plans to address the patient’s changing needs, ensuring steady improvement.
Adapting the Treatment:
As strength and mobility increase, exercises become more challenging to promote continued improvement. If obstacles arise, the treatment plan is adjusted accordingly to tackle them effectively.Introducing Advanced Techniques:
Depending on recovery progress, physiotherapists may incorporate advanced exercises, musculoskeletal recovery therapy, alternative pain management strategies, or new therapy techniques to optimise recovery.Reassessing Goals:
Milestones are reviewed periodically to ensure they remain realistic. As recovery progresses, goals may shift to include returning to work, sports, or everyday activities.
Patient Involvement and Self-Management
Empowering patients to take an active role in their recovery ensures better outcomes and fosters a sense of ownership over their progress.
Active Role in Recovery:
Patients are encouraged to fully engage in their rehabilitation journey by following at-home exercises, attending all therapy sessions, and maintaining a positive outlook. This commitment significantly enhances recovery outcomes.Consistency is Key:
Committing to the home exercise plan is essential for progress. Even if improvements feel gradual, consistent effort builds the foundation for lasting recovery and helps overcome obstacles along the way.Proactive Communication:
Patients are urged to keep their physiotherapist updated about any concerns, such as new pain or difficulty with exercises. Timely feedback allows for immediate adjustments to the treatment plan, preventing setbacks.
By closely monitoring recovery, making necessary adjustments, and encouraging active participation, physiotherapists ensure a holistic and effective post-operative physiotherapy approach that helps patients rebuild confidence and achieve meaningful, lasting results.

Common Questions You Might Have
Recovering from surgery often brings up many questions, and it’s natural to want to understand the post-operative physiotherapy process better. This section answers some of the most frequently asked questions, helping you feel more informed and confident as you navigate your rehabilitation journey.
1. How Long Will My Post-Operative Physiotherapy Last?
The length of time you’ll need physiotherapy after surgery depends on several factors, and it can vary widely from patient to patient. Here’s what to keep in mind:
Typical Duration of Physiotherapy
Post-operative physiotherapy generally lasts anywhere from a few weeks to several months, depending on the complexity of the surgery and your recovery pace. In the early stages, the focus is on gentle mobility exercises and pain management to reduce stiffness and restore basic movement. As recovery continues, strength-building exercises and more advanced techniques are introduced to help restore full function. The timeline can extend to 3–6 months for surgeries like joint replacements, while less invasive procedures may require a shorter period.
Factors That Affect Duration
Several factors can influence the duration of post-operative physiotherapy:
Surgery type:
More invasive procedures, such as joint replacements, typically require longer rehabilitation compared to less complex surgeries like soft tissue repairs.Age:
Older patients undergoing physiotherapy for the elderly may experience slower recovery due to natural ageing and potential health conditions, such as arthritis, that can delay healing.Pre-surgery fitness:
Patients in better physical condition often heal faster, as their muscles and joints are more resilient.Commitment:
Consistency with prescribed exercises is key to progressing more quickly, enabling your physiotherapist to make necessary adjustments.Complications:
Issues like infection or delayed healing can extend recovery, potentially requiring additional sessions to address.
Progression and Adjustments
Your post-operative physiotherapy plan will adjust based on your progress. Early on, the focus will be on restoring your range of motion and managing pain. As you improve, exercises will become more intense, incorporating strength-building tasks. Your physiotherapist will regularly assess your mobility, strength, and pain levels, adjusting goals as needed. The duration of post-operative physiotherapy depends on factors like the type of surgery, your health, and your commitment to recovery. Your physiotherapist will guide you through each stage, ensuring your recovery aligns with your body’s healing process.
2. Will Physiotherapy Hurt After Surgery?
It is important to understand how physiotherapy may impact you in the early stages of recovery. While post-operative physiotherapy is designed to support healing, it’s natural for patients to wonder whether they’ll experience pain during treatment. Let’s explore what to expect in terms of discomfort, how pain is managed, and when it’s vital to seek further advice.
Pain Management
Some discomfort during post-operative physiotherapy, especially in the early stages, is normal as your body heals. Stiffness or tenderness is part of the rehabilitation process and is usually temporary. As tissues heal and muscles are reconditioned, mild discomfort may indicate that your body is adapting and rebuilding strength. Over time, this discomfort should decrease, with noticeable improvements in mobility and reduced pain. The goal is steady progress, avoiding overloading the body to prevent setbacks.
Pain Reduction Techniques:
Physiotherapists use various techniques to manage pain and keep discomfort tolerable, helping you progress in your recovery. Soft tissue methods like massage ease muscle tension and improve circulation, supporting healing. Depending on your recovery stage, heat can relax muscles and promote blood flow, while cold reduces swelling and inflammation. These approaches relieve muscle spasms and enhance healing. Your physiotherapist will customise these techniques to ensure comfort and effectiveness throughout your post-surgery physio journey.
When Pain is a Concern
Some discomfort is normal, but it’s important to distinguish between healing pain and signs of something wrong. If you experience any pain or discomfort, communicate openly with your physiotherapist. If an exercise causes significant discomfort, inform your physiotherapist immediately. They’ll adjust the treatment to suit your recovery and ensure it remains safe and effective.
Distinguishing Between Normal Discomfort and Abnormal Pain
Not all pain is the same, and it’s important to distinguish between what is a normal part of the healing process and what may signal potential complications.
Normal Discomfort:
Mild soreness or stiffness is typically a sign that your muscles and joints are adjusting to movement. It should lessen as you regain strength and mobility.Abnormal Pain:
On the other hand, sharp, intense pain or pain that lingers long after the session may signal complications, such as joint instability, inflammation, or infection. Report any unusual or worsening pain to your physiotherapist for adjustments or further evaluation.
When to Seek Further Evaluation:
If pain persists or you notice swelling, redness, or heat around the surgical site, it could signal inflammation or infection and should be addressed by your physiotherapist or surgeon. Reporting these symptoms promptly helps prevent complications and ensures appropriate care. Any sharp, persistent pain that doesn’t improve with rest or typical pain management should also be reported. This may require a reassessment of your recovery or additional treatment.
While some discomfort during post-operative physiotherapy is normal, it’s important to communicate openly with your physiotherapist. They can adjust your treatment plan to manage pain effectively and keep your recovery on track. If you experience abnormal pain, speak up immediately so adjustments can be made to avoid further issues.
3. Can I Continue My Normal Activities During Post-Operative Physiotherapy?
After surgery, many patients are eager to return to their usual activities, but the timeline depends on the type of surgery and your recovery. Following your physiotherapist’s guidance is crucial to avoid setbacks. Here’s an overview of what to expect and how to safely resume your normal activities.
Activity Modifications
After surgery, it’s important to avoid high-impact or strenuous activities like running, jumping, or lifting heavy weights to prevent strain on the healing area. Your physiotherapist will guide you on which activities to avoid during the early stages of rehabilitation.
In the early phases, post-operative physiotherapy focuses on gentle mobility exercises to restore function, increase range of motion, and reduce stiffness, all while protecting the surgical site.
Gradual Introduction of Activities:
As you recover and gain strength, your physiotherapist will gradually reintroduce activities, starting with lower-intensity exercises like walking or light stretching. The aim is to ease you back into your routine while monitoring for any pain or discomfort. Your physiotherapist will assess your response and adjust the plan as needed, ensuring safe and comfortable progress.
Movement-based Adjustments:
Depending on your surgery, some everyday activities may need to be modified during the early recovery stages. Movements like bending, squatting, or twisting—including restrictions following physiotherapy for shoulder pain—may be adjusted to protect the surgical area. Your physiotherapist will teach you techniques to reduce strain, such as bending at the hips instead of the knees after knee surgery. These temporary modifications support healing and prevent setbacks.
Return to Work
The timing of your return to work depends on your job’s physical demands and the type of surgery you’ve had. Office-based jobs without heavy lifting or strenuous activity often allow for an earlier return, while physically demanding roles may require a longer recovery. Adjusting your workspace for proper posture may be necessary if your job involves sitting or repetitive movements. Your physiotherapist can guide you on desk setup to support recovery. In some cases, a gradual return to work, starting with part-time hours or lighter tasks, may be recommended.
Return to Sports
Returning to sports is a gradual process that depends on your recovery and the type of surgery. Your physiotherapist at a sports injury clinic will assess when it’s safe to resume activities. For example, after knee surgery, you may start with walking or swimming before progressing to running, which often parallels approaches used in physio for knee pain. High-contact sports like football or rugby require more time for healing. Sport-specific exercises will help prepare you for movements like jumping and quick direction changes. Your physiotherapist will guide you through the process for a safe return to activity.
Clearance to Resume Normal Activity
Your physiotherapist will clear you to resume specific activities once you’ve reached the necessary strength, mobility, and overall fitness levels. They may approve activities like running, lifting, or more intense exercises when confident in your progress. Throughout your recovery, they’ll monitor your movement, strength, and comfort to ensure safe progress, addressing any setbacks before resuming potentially risky activities. As with any injury, a gradual return is essential for long-term health and healing. Your physiotherapist will guide you in reintroducing work and sports based on your recovery.
How Professional Physiotherapy Supports Your Recovery
Post-operative physiotherapy is essential for bridging the gap between surgery and complete recovery. It’s not just about managing pain but rebuilding strength, improving mobility, and restoring function. After surgery, your body may feel weak or stiff, but with the right physiotherapy plan, you can regain independence and return to a more active life. Collaborating closely with your physiotherapist is key to a successful recovery. Together, you’ll set realistic goals tailored to your needs. Whether returning to work or resuming physical activities, your physiotherapist will guide you at every step. Recovery takes time, but with patience, dedication, and consistent effort, you’ll gradually regain strength and confidence.
Remember, recovery is a joint effort. By following your treatment plan, staying consistent with exercises, and communicating openly, you’ll make steady progress toward a full recovery.
At Rehab & Beyond, we recognise that every recovery journey is unique. Our experienced team of rehab physiotherapists is dedicated to providing personalised care tailored to your needs, ensuring the most effective treatment for your recovery. We take a holistic approach, empowering you to achieve long-term health and well-being.
Are you ready to start your rehabilitation journey, or have questions about post-operative physiotherapy? We’re here to support you. Contact us today to learn how we can help you achieve a healthier, more active future.
